I'm on orthopaedics at the moment, so we'll start with a straightforward one:
(Nb, if anyone wants to critique how I write this up, please feel free. After a year out I've gotten a touch rusty in pretty much every area)
A 68-year-old Caucasian female presents to the ED with severe (9/10) left ankle pain. She stood up from a seated position, and her foot slid out from underneath her, resulting in an audible 'crack' from her ankle. She has been brought in in a wheelchair, as she is unable to weight-bear on the left side.
On inspection, the ankle and the dorsal aspect of the foot are severely swollen, but the foot is not grossly displaced. There are no lacerations or abrasions, and the colour and temperature of the left foot and ankle are normal. She has bimalleolar tenderness, but her foot and lower leg are non-tender. She is unable to actively perform any ankle or foot movements on the left side, and has lost sensation over the dorsum of the foot. She sustained no other injuries during her fall. She is otherwise well, and reported no abnormal symptoms prior to her fall. Her only significant history is of a radial fracture after a FOOSH 7/12 ago.
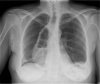
X-rays reveal a trimalleolar fracture.
1) List the bones and major ligaments involved in the ankle joint
2) What are some possible complications to watch for following this type of injury, and how would you monitor these?
3) What other injuries commonly co-occur with ankle injuries caused by rotational forces?
4) Management plan and rationale. Go. Include in your answer why surgery is/isn't likely to be required for this type of injury.
5) This is her second fracture in the past year. What are her risk factors for osteoporosis, and how (if at all) would you test her for it?
6) Both of her recent fractures occured following falls. List 5 possible factors which may have contributed to these falls, keeping in mind her demographic factors and the mechanism of the fall given in the vignette. Outline how you would go about determining which (if any) may have been responsible, and how these could be managed going forward.
I'm on my phone, so I can't be bothered typing out my answers. I'll edit them in later.
----
I'll give this a go even though I am going for JMP admission a few yrs down the track due to my own current health. Any feedback is greatly appreciated!

68YO WF presents to ED in W/C with c/o severe L ankle pain after fall. Pain score 9/10. Pt states stood up from a seated position, and her foot slid out from underneath her, resulting in an audible 'crack' from her ankle. NIL WBAT and ankle or foot movements on L side, NIL gross displacement, NIL Lac or abrasions, NIL other injuries.
On inspection, the ankle and the dorsal aspect of the foot are severely swollen, but the colour and Temp of the L foot and ankle are normal. Bimalleolar tenderness noted, but LF and LLL are non-tender. Pt has loss of sensation over the dorsum of LF.
Otherwise well. Reported no abnormal symptoms prior to her fall.
PMH:
Radial fracture after a FOOSH 7/12 ago.
Reflexes normal on right side but reduced movement on L side due to pain.
XR LF and L ankle reveals a trimalleolar fracture.
1) Main bones: talus (in the foot), and the tibia and fibula (in the leg)
Ligaments: medial ligament (or deltoid ligament), lateral ligament, Anterior talofibular, Posterior talofibular, Calcaneofibular.
2)
blood clots in the legs—U/S, pt history, D-dimer, MRI, CT, heart/lungs, legs for warmth, swelling, bulging veins, or changes in skin colour.
infection— FBC
malunion— XR, CT, MRI.
osteoarthritis—pt history/family history, swelling and tenderness of the joints, loss of movement in specific joints, or visible joint damage such as bony growths in the surrounding area, Joint aspiration or arthrocentesis, XR, MRI.
3) Tarsal Tunnel Syndrome, Peroneal Tendonitis, Sinus tarsi syndrome, Tibialis Anterior Tendonitis.
4) Plan:
Surgery not suitable for this pt due totoo high of a risk due to other health conditions.
Discharge with advice re analgesia, ankle overuse, falls education and osteoporosis.
Organise PT outpatient appt re suitable exercises
Repeat XR in 6/12 to check healing
Discharge
5) Risk factors:
smoking—GATS survey
alcohol— survey
low weight— BMI
low physical activity— GPAQ, pt questioning.
poor nutrition—NNS
Testing for osteoporosis:
Bone density test.
6) 5 possible factors which may have contributed to these falls:
· Unsafe mobility-- Poor balance and decreased strength
· Visual impairment-- Vision prescription that is out of date
· Medications-- Side effects of some medication
· Home hazards—clutter, poor lighting, unsafe bathrooms, loose mats, holes in carpet, slippery floors, hoses and pets.
· Chronic conditions- long term undiagnosed condition such as osteo/rheumatoid arthritis.
Management: Falls education booklet/talk, OT R/v of house, med R/V, optometrist to R/V prescription, GP R/V to see if undiagnosed chronic condition and any associated hearing or BP/postural drop problems that could be causing poor balance.